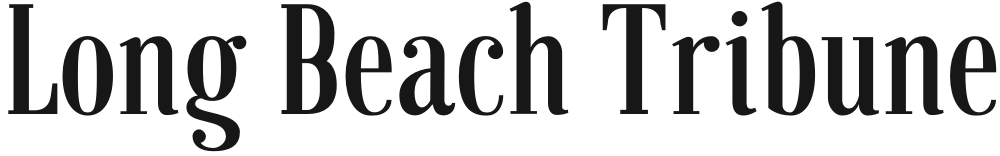Recent genetic study shows that people with one specific blood type are more likely to develop serious Covid-19 condition compared to others
Following the Covid-19 winter wave that resulted with new daily record high numbers driven by the Omicron variant, America is currently in a calmer period with low and steady numbers. Hospitals are finally relived by the several-month-long pressure by the virus and almost every American now lives in an area where they can stop wearing masks indoors, as per the updated CDC’s mask guidelines that also apply for schools.
According to the New York Times’ Covid-19 tracker, America on March 20 added a total of 7,844 new Covid-19 cases nationwide. The declining trend is confirmed by the 14-day average number that now dropped to 29,905 cases per day which is 33% less compared to the previous 14-day average. In addition, there are 16,465 people currently hospitalized due to Covid-19 in America, which is 57% drop in the 14-day change category.
Since the start of the pandemic more than two years ago, health experts and scientists are constantly working to determine how different factors might affect the severity of the illness in those who get infected with Covid-19. So far, dozens of studies have found age and previous health condition to be two of the most impactful factors that play a role in developing severe Covid condition and Covid-related deaths.
Since not much is known about the deadly virus, there are numerous undergoing studies which should reveal more details about corona that will later help the health experts and health officials in providing better treatment and developing more effective vaccines in battling the virus. One such recent study revealed that blood type might play a role in the severity of one’s COVID-19 symptoms.
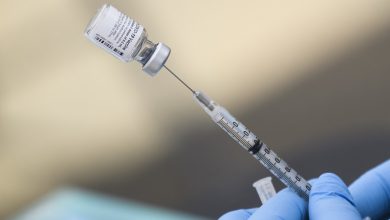
According to a paper published earlier this month in the journal PLOS Genetics, scientists screened more than 3,000 blood proteins to determine which ones actually caused positive or adverse COVID-19 outcomes. “Severity” was, in this context, defined as a COVID-19 case in which a patient required hospitalization and/or respiratory assistance — or actually led to the patient’s death. By the time the scientists were done, they had whittled the number of potential protein suspects down to just over a dozen — and one of them happens to be a protein that determines your blood type.
The study revealed that people with Type A blood are more likely to get severely sick from COVID-19. However, this doesn’t mean that this group of people should immediately panic.
“Our study does not link precise blood group with risk of severe COVID-19 but since previous research has found that proportion of people who are group A is higher in COVID-19 positive individuals, this suggests that blood group A is more likely candidate for follow-up studies,” Christopher Hübel from King’s College London, co-last author on the study, told New Atlas.
While the study shows clear correlation between Type A blood and the Covid-severe condition, the paper’s authors reminded everyone there still are plenty of other things and factors that will most likely affect the severity of the illness more compared to the blood type. Obesity, age, pre-existing immune diseases and general health condition are just few of the factors with higher impact on Covid-19 severity compared to the type of blood.
Previously, a study published in the New England Journal of Medicine (NEJM) has showed that people with type A blood are associated with having a 45% higher risk of contracting, but the latest study published in the journal PLOS Genetics has offered the clearest insight to date into the causal relationship between blood type and COVID-19 severity.